Description
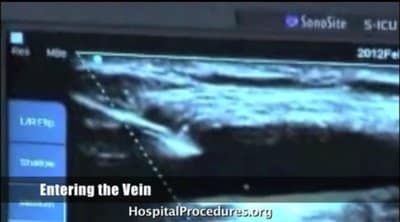
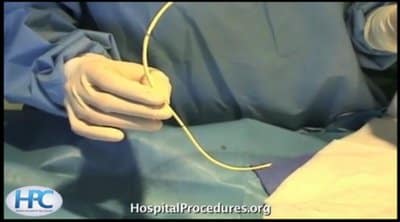
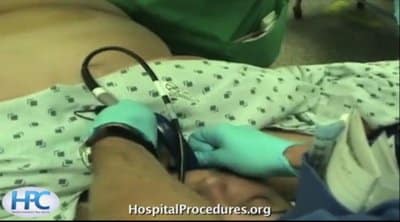
This video demonstrates ultrasound guided peripheral venous catheter insertion. A useful hospital and emergency procedures, ultrasound guided peripheral line insertion is shown step by step. Clinical pearls and common pitfalls associated with peripheral lines are discussed in detail. The video is not downloadable but may be accessed indefinitely by internet from any computer, smart phone, or tablet. Click below to preview the ultrasound guided peripheral IV video.


Reviews
There are no reviews yet.