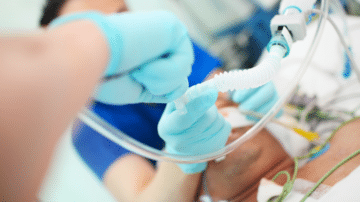
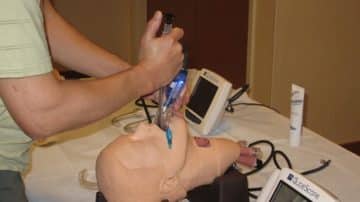
Unexpected difficulties in intubation are more common than one might think, with an incidence rate that varies from 0.1% to 10.1%. They pose a higher risk of injury, with repeated attempts leading to severe complications that include edema, increased gastric…
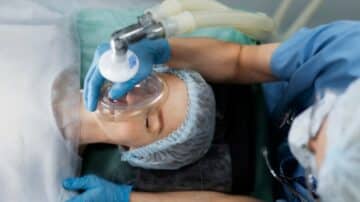
Read MoreEndotracheal intubation can occur in up to 60% of critically ill patients. Though common, the procedure comes with significant risks. If multiple attempts are made to secure the airway, it may contribute to patient morbidity. Using the right laryngoscope can…
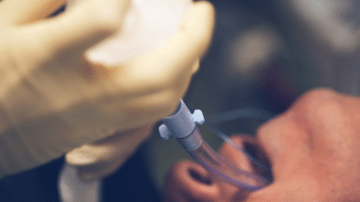
Read MoreMore than 80% of critical care patients lack the capacity to make decisions regarding the withholding or withdrawal of treatments. Some don’t have a surrogate decision-maker or an advance directive. How should ICU clinicians make treatment decisions for these patients?…
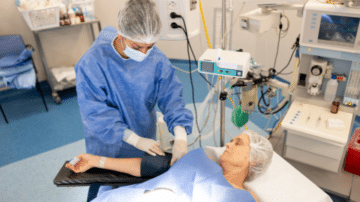
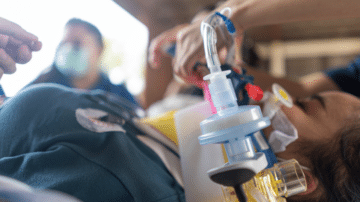
Read MoreProcedural sedation and analgesia (PSA) is a widespread practice that allows the patient to maintain oxygenation and independent airway control while being in a sedated or dissociative state. When should PSA be used and avoided? What are the various levels…
Read MoreFive to 15% of trauma patients arrive in emergency rooms in shock. From June 2020 to April 2022, less than 10% of admitted patients met the criteria for multifactorial shock in the early phase, putting them at a significantly higher…
Read MoreNearly half of adult Americans are obese, putting them at higher risk for several health issues. Should they be admitted for treatment, this patient group is slightly more challenging to intubate than others (11% vs. 7%). The process requires clinicians’…
Read MoreHemodynamic monitoring is used to assess the functional characteristics of the cardiovascular and circulatory systems. In critical care patients, it guides the medical team in preventing or treating organ failure while improving patient outcomes. Though the extent of its benefits…
Read MoreWhich is better for critically ill patients—direct laryngoscopy (DL) of video laryngoscopy (VL)? This question has ignited an intense debate within academic, emergency medicine, and critical care communities as 13 to 20 million intubations are performed annually in the United…
Read MoreMore Tags – Dialysis Catheter
In 2010, 2.6 million individuals received renal replacement therapy. Most of them were also receiving hemodialysis treatments. That number has since grown to 4 million, making knowledge of the procedure vital for healthcare practitioners. Though catheter insertion is an important…
Read MoreMore Tags – Breath Stacking
Mechanical ventilation (MV) is necessary for sustaining life among patients experiencing respiratory failure, cardiopulmonary arrest, severe neuromuscular disorders, upper airway obstruction, and those with unprotected airways. While mechanical ventilation can save lives, reduce mortality and lower healthcare costs, breath stacking…
Read MoreVideo laryngoscopy (VL) is a valid technique for difficult airway management in awake patients. But for patients with a history of difficult mask ventilation or intubation, awake fiberoptic intubation is widely considered the gold standard. It provides a clear visualization…
Read MoreAscites, the abnormal buildup of protein-containing fluid in the abdominal area, is a common complication of cirrhosis. It can also develop due to heart failure, cancer, kidney disease, and a few other conditions. Performing a paracentesis procedure could aid in…
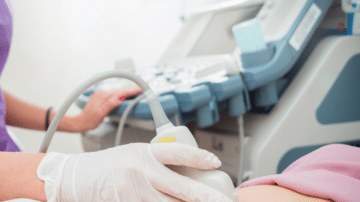
Read MoreMore Tags – ultrasound of spine
Longitudinal spine ultrasound with linear array probe Also known as a “spinal tap,” a lumbar puncture is used to diagnose life-threatening diseases, administer medications, and measure intracranial pressure. An estimated 360,000 of these procedures are performed annually in the U.S.…
Read MoreA central venous catheter (CVC), also called a central line, is similar to an intravenous line but is more often used for critically ill patients who require longer treatments. It is a common bedside procedure performed using sterilize equipment. It…
Read MoreOver 400,000 Americans are intubated in emergency settings annually for various reasons—about 12.7% of them are unsuccessful on the first attempt. Failure to intubate the trachea on the first try occurs in up to 20% of cases. To make matters…
Read MoreCategories
- ACLS (1)
- Arterial line (33)
- Cardiovascular diseases (77)
- Central line (55)
- Chest Tube (39)
- Dermatology (4)
- Emergency Procedures (138)
- Endocrinology (6)
- Endotracheal Intubation (36)
- Events (24)
- FAST Exam (12)
- Featured (112)
- Featured Procedure (42)
- Gastrointestinal diseases (32)
- Ginecology (3)
- Glidescope Intubation (21)
- Hematology (33)
- Hospital Procedures (85)
- Infections (32)
- Intraosseous line (8)
- King Tube (27)
- Laryngeal Mask Airway (18)
- Lumbar Puncture (36)
- Mechanical Ventilation (34)
- Medical General (95)
- medical procedures (258)
- Needle Decompression (6)
- Nephrology (11)
- Neurological diseases (12)
- Oncology (4)
- Paracentesis (32)
- Pericardiocentesis (3)
- Procedural Sedation (19)
- Respiratory diseases (85)
- RUSH Exam (8)
- Thoracentesis (37)
- Traumatology (24)
- Travel (27)
- Ultrasound-Guided Peripheral IV (13)